

Joint replacement surgery has become a common way to restore joint function and improve quality of life. The long-term durability and safety of artificial joints are primary concerns for both doctors and patients. Among the many influencing factors, material plays a decisive role. Currently, the main clinical materials for artificial joints are metals, polymers, and ceramics. Each has its own cons and pros, then, which material is best?
We must first comprehend the biological and mechanical specifications that a successful artificial joint material should fulfill before making a comparison of these materials.
Metal materials offer exceptional strength and toughness. They are primarily used as the load-bearing framework for artificial joints, such as the femoral stem, femoral condyles, and the base of the acetabular cup.
Among all metal materials, stainless steel was the first used for artificial joint prostheses due to its reasonable corrosion resistance and mechanical strength. However, stainless steel contains elements like Nickel, which can be teratogenic, making it unsuitable for long-term implantation. Furthermore, stainless steel itself is not bioactive and struggles to form a stable, strong bond with bone tissue. Consequently, stainless steel has gradually been replaced by other alloys in joint implants.
Current mainstream materials include titanium alloys, cobalt-chromium alloys, and tantalum.
Titanium alloy offers excellent biocompatibility, and its elastic modulus is closer to that of human bone, effectively reducing stress shielding. More importantly, it supports osseointegration, allowing bone cells to grow directly on its surface, forming a strong bond. The first titanium alloy used for artificial joints was Ti-6Al-4V. It possesses good heat resistance, strength, plasticity, toughness, formability, weldability, corrosion resistance, and biocompatibility. Ti-6Al-4V is often used to manufacture femoral stems and acetabular cups that require strong integration with bone. However, its wear resistance is relatively poor, so it is not typically used for the articulating bearing surface.
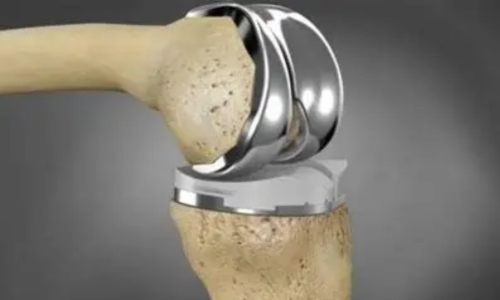
Cobalt-chromium alloy is a hard alloy resistant to various types of wear, corrosion, and high-temperature oxidation, and CoCrMo alloy is the widely used. Its greatest advantage is the extremely high wear resistance and strength. Therefore, it is commonly used in areas subject to high wear and stress, such as the femoral condyles in knee joints and the femoral head in hip joints.
This is a relatively new type of orthopedic implant material. And now it is recognized as an ideal orthopedic implant material with many advantages.
1)Its porous structure resembles the trabecular structure of cancellous bone, thence it is highly suitable for bone ingrowth.
2)Its elastic modulus matches that of the surrounding bone tissue and avoids stress shielding.
3)Furthermore, porous tantalum is chemically stable in bodily fluids, exhibiting excellent biocompatibility.
The traditional methods for manufacturing artificial joints are forging, casting, and precision machining. These are mature, stable processes capable of producing metal components with uniform properties and high density.
Simultaneously, 3D printing technology is gaining increasing attention. It uses fine metal powders as raw materials, such as Ti-6Al-4V and CoCrMo powder. Layers of powder are selectively melted by a laser or electron beam, precisely building complex three-dimensional structures. 3D printing can create intricate geometries that are difficult or impossible to achieve with traditional methods. It also allows precise control to create porous structures with high porosity and interconnected pores, which is crucial for promoting bone ingrowth and achieving biological fixation – a structure very difficult to achieve with traditional forging/casting.

Metal powder, as the raw material for 3D printing, plays a vital and growing role in manufacturing critical porous structures and customized components. Stanford Advanced Materials (SAM) offers a wide range of high-performance spherical alloy powders suitable for medical implants.
Polymer materials primarily serve as the "cartilage" in artificial joints, acting as the articulating liner. And it forms the bearing couple with a metal or ceramic femoral head.
1. Polymethylmethacrylate (PMMA)
It is commonly known as "bone cement." It does not form the joint surface itself but acts as a fixation medium, which anchors prosthetic components within the medullary canal. It provides immediate fixation through mechanical interlock. However, the heat generated during its polymerization and potential monomer residue pose certain risks.
2. Ultra-High-Molecular-Weight Polyethylene (UHMWPE)
This is currently the gold standard material for manufacturing acetabular liners and tibial inserts. Compared to standard polyethylene, UHMWPE has extremely long molecular chains, which make it high impact resistance, wear resistance, and a low friction coefficient.
3. Highly Cross-linked Polyethylene (XLPE)
Building upon UHMWPE, XLPE is processed using high-energy radiation followed by thermal treatment, creating additional cross-links between molecular chains. This process significantly enhances the material's wear resistance. And the wear rate is reduced by approximately 90% or more compared to conventional UHMWPE.
Unlike everyday ceramics, artificial joint ceramics are made from high-purity alumina, zirconia, or composite ceramics. These advanced ceramics are sintered under high temperature and pressure, making them extremely hard and smooth.
The ceramic-on-ceramic interface is particularly suitable for young, active patients. However, it carries potential risks, namely brittle fracture and the possibility of audible squeaking. Modern manufacturing techniques have made fracture incidence extremely rare.
Returning to the initial question: which material is best? There is no absolute answer. The choice depends on the patient's age, activity level, overall health, and the specific joint being replaced.
|
Property |
Metal |
Polymer |
Ceramic |
|
Strength/Toughness |
Excellent |
Good |
Excellent, but high brittleness |
|
Wear Resistance |
Excellent (CoCr) |
Excellent (XLPE) |
Exceptional |
|
Biocompatibility |
Excellent (Ti Alloy) |
Good |
Excellent |
|
Osseointegration |
Excellent (Ti/Ta) |
None |
None |
|
Main Application |
Load-bearing structures |
Articulating liners |
Articulating surfaces |
1) Metal-on-Highly Cross-linked Polyethylene is the most widely used and technologically mature combination globally, because it balances performance, safety, and cost. This is suitable for the vast majority of patients.
2) Ceramic-on-Highly Cross-linked Polyethylene is currently the fastest-growing combination. It combines the durability of a ceramic head with no risk of squeaking or fracture. It is thence an excellent option for young, active patients.
3) Ceramic-on-Ceramic provides the most superior wear resistance. It is the ultimate choice for young patients with a long life expectancy and very high activity demands. However, it requires higher surgical precision and carries the potential for audible squeaking and a very low risk of fracture.

United States




